
Healthy, well-maintained gums provide the foundation for strong adult teeth. Of course, taking care of your gums does more than just maintain stability for your teeth. Good dental care also helps prevent gum disease, which can cause oral health issues and can aggravate heart problems. No matter your age, you can take simple steps every day to improve the health of your gums and teeth. Start with these five essentials; then, ask your dentist what other steps you can take to protect your gums.
1. Stay On Top of Brushing and Flossing
Dentists recommend brushing your teeth at least twice a day after meals and flossing once a day. If you can, try brushing your teeth three times a day. Health officials in many countries suggest brushing your teeth before breakfast and about an hour after each meal. Avoid brushing your teeth immediately after you eat, especially if you’ve had acidic foods. You can floss at any time of the day; choose the same time every day to make flossing a habit.
2. Avoid Mouthwash with Alcohol
Many over-the-counter mouthwashes contain an enormous amount of alcohol. Avoid using these rinses as they can dry out the mouth and gums, leading to discomfort and encouraging the growth of bacteria. Opt for all-natural or alcohol-free mouthwashes instead and use them at least twice a day.
3. Eat A Healthy, Well-Balanced Diet
The American Dental Association and other medical groups have launched educational campaigns to explain that eating well can improve oral health. Choose plenty of fresh fruits, vegetables and whole grains. Avoid eating too many sweets as they can damage teeth and encourage the growth of bacteria.
4. Keep Your Tongue Clean
Your tongue is a great breeding ground for bacteria. To boost overall oral health, scrape your tongue twice every day with a tongue scraper. A specialized scraper will remove more bacteria than a regular toothbrush.
5. Stay Well-Hydrated
Drinking plenty of water helps your mouth and gums stay hydrated, which in turn helps control bacteria. If you’re in an office environment all day, try to drink one glass of water every hour. If you’re active, you’ll need to drink extra water to protect your gums and stay hydrated.
Remember that choosing a dentist in your area for regular checkups and cleanings is the cornerstone of good oral health. Your dentist can complete yearly oral health screenings and alert you to any early signs of gum disease. Starting a gum care regimen today is a great way to improve oral health and offset any early indicators of disease.

Dental implants are used to replace damaged or missing teeth. Unlike bridges and dentures, dental implants are permanent tooth replacements that maintain the appearance, comfort, and function of your natural teeth. This makes them a much preferred tooth replacement alternative amongst patients concerned, not only with the aesthetics of their smile, but the comfort and upkeep of their replacement teeth. Most patients with missing or damaged teeth are candidates for dental implants, presuming they are in good health. Because dental implants require surgery, your periodontist must assess your individual circumstances to determine if you are healthy a viable candidate for the procedure.
Dental implant surgery requires multiple sessions, but the procedure is widely practiced and has become highly routine among most dental professionals. As with any surgical procedures, there are some risks that should be considered, but you can discuss these with your dentist or periodontist to take all factors into consideration.
When performed by an expert periodontist, the dental implants procedure is fast, relatively painless, and effective. And with proper aftercare and consistent upkeep, any of the procedure’s potential risks is drastically minimized.
Potential Risks of Dental Implants
Dental implants have been used by periodontists for over 30 years, so the procedure has a long history of success. While dental implant surgery is considered to be one of the safest and most predictable dental procedures, here are some factors to consider when electing to receive dental implants:
● Infection at the implant site. Infection at the site of any surgical procedure is something any medical professional would caution their patients about. With dental implants specifically, the procedure involves inserting the implant into the bone socket of the missing tooth–that is, into the jawbone itself. Periodontists take every precaution to keep the area sterile and minimize the risk of infection, and if you follow aftercare instructions thoroughly, you reduce the risk of infection post procedure.
● Damage to surrounding structures. Because the procedure involves drilling into the jawbone, in rare occasions, there is the risk of damaging the bone, the surrounding teeth, nerve endings, or even blood vessels. If your own jaw is not strong enough to support dental implants, you may require bone grafts to reinforce the structure of your jaw, and this also has the potential to do damage to the existing area. But such instances are rare in procedures handled by skilled periodontists.
● Sinus problems. When dental implants are placed in the upper jaw, there is the potential for the implant to protrude into the sinus cavity and cause problems with your sinuses. Periodontists avoid this with comprehensive examinations before the procedure. X-rays, CT scans, and molds of your teeth all go into helping your periodontist determine the precise shape, size, and structure of your jaw to help them place the implant directly.
The Advantages of Safe Dental Implants
There are a myriad of advantages to choosing dental implants, both aesthetically and functionally. They look and feel natural, providing you with a health replacement for your natural teeth that gives you a radiant smile. They are also permanent, unlike bridges and dentures, so as long as you take regular care of them (as you would with your natural teeth), you do not have to worry about removing them daily or taking extra steps to care for them beyond brushing and flossing. There is no impediment to your speech, and very little pain after the procedure, and with dental implants, there are no restrictions to your diet.
In fact, according to the American Academy of Implant Dentistry, dental implants go above and beyond mere tooth replacement insofar as they actually stimulate bone growth. The titanium that the implants are made of fuses with your natural bone in a process called osseointegration. This not only offers stability for the implant, but as more bone grows to fuse with the titanium, your jawbone is strengthened, and this can provide needed reinforcement against future tooth loss.
All in all, dental implant surgery is a safe procedure with a wide array positive benefits for patients. If you are considering dental implants, it is important to research not only the procedure but also the periodontist you want to work with. Some dentists, like Dr. Jan Linhart, have a periodontist on staff, but if they don’t, they can likely recommend one. Remember, you are in control of your oral health. Be active in your research and explore all your options for ensuring the safest way to attain the smile you’ve always wanted.
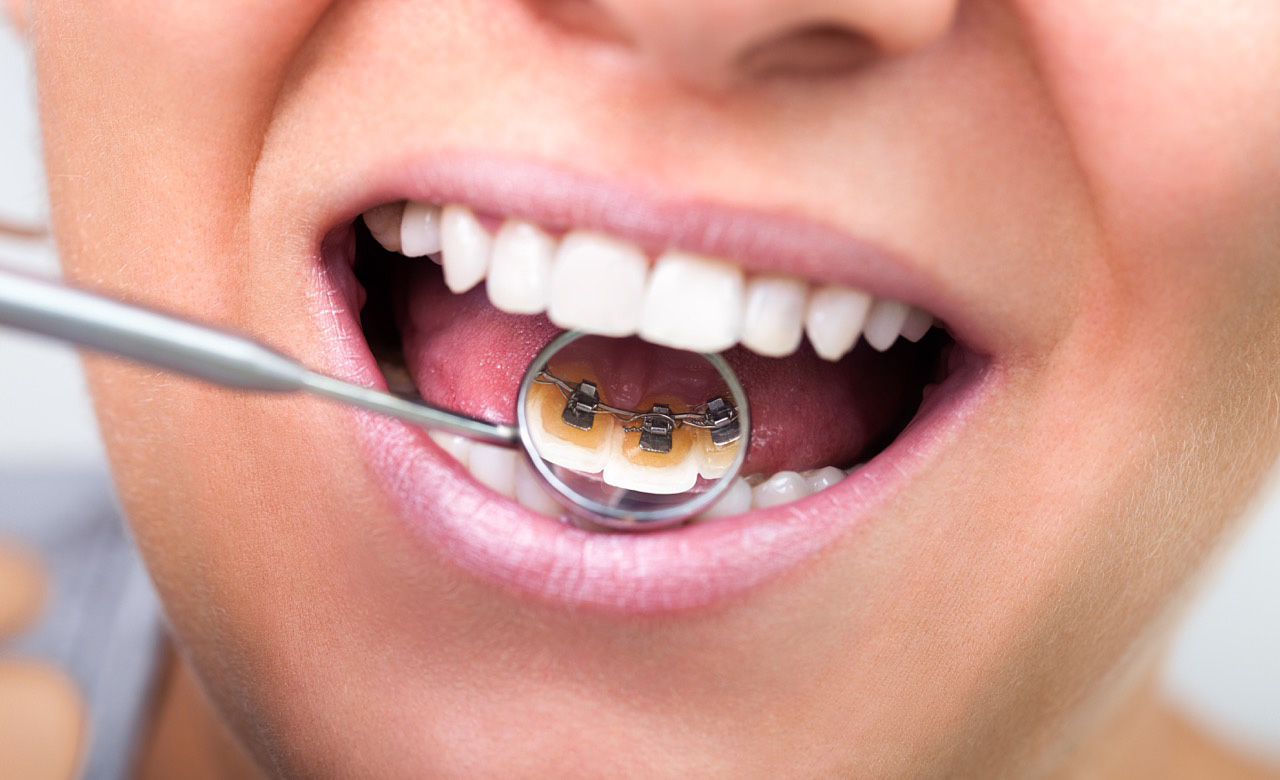
Nowadays, with so many alternatives to traditional braces–such
as Invisalign or porcelain veneers–orthodontic patients have a
wide range of options to fit their individual needs. While traditional braces are effective and still widely used by orthodontists
to correct misaligned teeth, newer technologies have made some orthodontic
treatments faster, more comfortable, and more aesthetically pleasing.
iBraces are one such treatment that have grown
in popularity among patients because they offer an efficient, virtually
invisible alternative to conventional braces. iBraces work very similarly to
traditional braces, using brackets and wires to straighten teeth, but they are
the only orthodontic braces that are 100% customizable. What sets iBraces apart
as a truly unique and individualized orthodontic solution?
The iBraces Difference
iBraces are not visible on the front side of your teeth.
Instead, each bracket is anchored to the back of each individual tooth. The
brackets are smaller than those used in traditional braces, so they don’t
interfere with speech, and they are contoured to perfectly hug the lingual
(tongue-side) surfaces of your teeth. While this makes more comfortable
conventional braces, it isn’t the only thing that makes iBraces unique.
The secret to iBraces is the fact that each brackets is made specifically to each individual tooth.
This not only ensures maximum comfort and efficiency, but makes for a
completely customized set of braces that is tailored to provide the ideal amount
of corrective movement your teeth need. The iWires that connect each bracket
and are tightened to straighten teeth are shaped using robotic technology. This
ensures that the wires are “programmed” for your specific treatment plan,
allowing them to produce the best outcome.
iBraces are quicker than regular braces, though the specificity
of iBraces prescriptions means that the length of treatment varies from patient
to patient. Regardless, if you and your orthodontist determine iBraces are
right for you, you can expect to be finished with your treatment faster than if
you had gone with traditional braces.
iBraces with Doctors Linhart & Mathrani
At Linhart Dentistry, Dr.
Rohini Mathrani is an exceptionally skilled orthodontist and our
iBraces specialist. iBraces is typically a viable option for most adults and
adolescents who have their permanent teeth, but if you have any special
circumstances. Dr. Mathrani can recommend the best solution for you. to learn
more about iBraces and other orthodontic treatments, contact
Linhart Dentistry today to schedule an appointment.
Dental implants are used to replace damaged or
missing teeth. Unlike bridges and dentures, dental implants are permanent tooth
replacements that maintain the appearance, comfort, and function of your
natural teeth. This makes them a much preferred tooth replacement alternative
amongst patients concerned, not only with the aesthetics of their smile, but
the comfort and upkeep of their replacement teeth. Most patients with missing
or damaged teeth are candidates for dental implants, presuming they are in good
health. Because dental implants require surgery, your periodontist
must assess your individual circumstances to determine if you are healthy a
viable candidate for the procedure.
Dental implant surgery requires multiple sessions, but the
procedure is widely practiced and has become highly routine among most dental
professionals. As with any surgical procedures, there are some risks that
should be considered, but you can discuss these with your dentist or periodontist
to take all factors into consideration.
When performed by an expert periodontist, the dental implants
procedure is fast, relatively painless, and effective. And with proper
aftercare and consistent upkeep, any of the procedure’s potential risks is
drastically minimized.
Potential Risks of Dental Implants
Dental implants have been used by periodontists for over 30
years, so the procedure has a long history of success. While dental implant
surgery is considered to be one of the safest and most predictable dental procedures,
here are some factors to consider when electing to receive dental implants:
●
Infection at the
implant site. Infection at the site of any surgical procedure is something
any medical professional would caution their patients about. With dental
implants specifically, the procedure involves inserting the implant into the bone socket of the missing
tooth–that is, into the jawbone itself. Periodontists take every precaution to
keep the area sterile and minimize the risk of infection, and if you follow
aftercare instructions thoroughly, you reduce the risk of infection post procedure.
●
Damage to
surrounding structures. Because the procedure involves drilling into the
jawbone, in rare occasions, there is the risk of damaging the bone, the
surrounding teeth, nerve endings, or even blood vessels. If your own jaw is not
strong enough to support dental implants, you may require bone grafts to
reinforce the structure of your jaw, and this also has the potential to do
damage to the existing area. But such instances are rare in procedures handled
by skilled periodontists.
●
Sinus problems.
When dental implants are placed in the upper jaw, there is the potential for
the implant to protrude into the sinus cavity and cause problems with your
sinuses. Periodontists avoid this with comprehensive examinations before the procedure. X-rays, CT scans,
and molds of your teeth all go into helping your periodontist determine the
precise shape, size, and structure of your jaw to help them place the implant
directly.
The Advantages of Safe Dental Implants
There are a myriad of advantages to choosing dental implants,
both aesthetically and functionally. They look and feel natural, providing you
with a health replacement for your natural teeth that gives you a radiant
smile. They are also permanent, unlike bridges and dentures, so as long as you
take regular care of them (as you would with your natural teeth), you do not
have to worry about removing them daily or taking extra steps to care for them
beyond brushing and flossing. There is no impediment to your speech, and very
little pain after the procedure, and with dental implants, there are no
restrictions to your diet.
In fact, according to the American Academy of Implant Dentistry, dental
implants go above and beyond mere tooth replacement insofar as they actually
stimulate bone growth. The titanium that the implants are made of fuses with
your natural bone in a process called osseointegration. This not only offers
stability for the implant, but as more bone grows to fuse with the titanium,
your jawbone is strengthened, and this can provide needed reinforcement against
future tooth loss.
All in all, dental implant surgery is a safe procedure with a
wide array positive benefits for patients. If you are considering dental implants, it is important
to research not only the procedure but also the periodontist you want to work
with. Some dentists, like Dr. Jan Linhart, have a periodontist
on staff, but if they don’t, they can likely recommend one.
Remember, you are in control of your oral health. Be active in your research
and explore all your options for ensuring the safest way to attain the smile
you’ve always wanted.
The dental implant procedure is a safe and
permanent alternative to bridges and dentures as a replacement for missing
teeth. Periodontists
(specialists in gums and the bone structures that support your teeth) can
perform the procedure on anybody who is missing one or more teeth, as long as
they are in good health and have generally good oral hygiene.
In the 1950’s, Professor Per-Ingvar Branemark discovered that
living bone can fuse with titanium oxide to become an inseparable combined
structure. This is known as osseointegration, and it was the discovery that
paved the way for dental implants. Essentially, dental implants are small
titanium cylinders that are inserted into the jawbone where the missing tooth
is. The titanium acts as the root of the tooth, and once it fuses to the bone,
it becomes a permanent anchor for a false tooth that looks, feels, and works
exactly like your natural teeth.
The procedure for dental implants requires multiple sessions,
and can typically take around 18 months to complete. Despite the amount of
time, and the level of involvement with the jawbone and gums, it is generally
considered to be a very safe procedure. When it comes to the implants
themselves, there are two types of dental implants: endosteal and
subperiosteal.]
Endosteal Dental Implants
Endosteal implants are the most common type of dental implants
used for the procedure, and are generally used for patients who have no special
circumstances or prohibitive conditions. In other words, if you are healthy
overall and don’t have any complications or other factors affecting your oral health,
your periodontist will likely use endosteal implants.
Endosteal implants are usually shaped like screws, cylinders,
or blades. They are surgically implanted directly into the jawbone during phase
one of the procedure. In the office, your periodontist will use local
anesthesia to numb the area before placing the implant. The implant is then
left alone for three to six months while osseointegration occurs and the
titanium fuses to your bone, thus ensuring a solid foundation for the
prosthetic tooth.
If you are concerned with the aesthetics of a missing tooth, or
difficulty chewing or speaking, ask your periodontist about temporary bridges
or dentures that can be used to cover the implant during phase one. Phase two
of the implant procedure involves creating a new tooth that is attached to the
titanium anchor. An endosteal implant can hold one or more prosthetic teeth,
depending on your need.
Subperiosteal Dental Implants
Subperiosteal implants are an alternative to endosteal implants
for patients who would not otherwise be a candidate for traditional dentures.
Patients who have weaker jawbones, or who have minimum bone height (a shallow
jawbone that could not support an endosteal implants) may need subperiosteal
implants.
Subperiosteal implants are titanium frames that are fitted over the jawbone, as opposed to inserted
into it. They are implanted just below the gum tissue, and as the gums heal,
osseointegration occurs, fusing the frame to the bone. Metal posts attached to
the frame protrude through the gums, and this is where the prosthetic tooth is
mounted. The fused frame acts as an anchor in the same way that the endosteal
cylinders do.
As with endosteal implants, subperiosteal implants usually
require a two-phase process that occurs over several months: the placement of
the implant, followed by the mounting of the prosthetic tooth. However, recent
developments have lead to an alternative method for both types of implants.
Depending on the patient’s oral health, the number of teeth involved, and the
position of the teeth, your periodontist may be able to install the dental
implant in one whole piece, during a single session.
—
If you have fractured or missing teeth and are considering your
options, ask Dr. Linhart about dental implants. More often than not, you will
be a candidate for the procedure, which offers a convenient and lasting
solution to bridges or removable dentures. As with any surgical procedure,
there may be some risks involved, depending on your individual circumstances. Linhart Dentistry can work with you to assess all your options and determine the
best way to restore your smile.
PearlInBrite is a proprietary teeth whitening
system pioneered by Dr. Jan Linhart to speed up the process so
that patients experience results immediately. In as little as one session (two
hours), patients can expect a 9-10 shade change in the color of their teeth, depending
on the degree of previous staining.
PearlInBrite is a laser whitening system, which, like all
whitening procedures, use peroxide to bleach the teeth. With ordinary laser
teeth whitening, the molecules in the peroxide are “excited” by laser energy to
break down the stains and whiten teeth. Dr. Linhart’s procedure, however, uses two different lasers instead of one, and
three laser-specific gels to achieve an optimum white.
PearlInBrite Laser Tooth Whitening is far more effective than
any other tooth whitening system. However, for results to last, patients must
maintain proper dental hygiene and continue to brush and care for their teeth
on a regular basis. How can you make the most of your PearlInBrite experience
after the procedure? Here are 5 aftercare tips to make your teeth whitening
treatment last longer.
1.) Brush, Floss, and Care for Your Teeth
Regularly
This is important to the overall state
of your oral health–not just maintaining the whiteness of your teeth. However,
proper dental hygiene does remove plaque and debris that can stain your enamel,
thus preserving your bright new smile. Brushing your teeth after every meal is
ideal, although twice a day is more than efficient. You should also be flossing
once a day, and consider adding mouthwash to your daily regimen. Consult with
your dentist if you have any questions about specific whitening toothpastes or
similar at-home products.
2.) Consider Using PearlInBrite
Whitening Enhancer
What better way is there to maintain
the results of your PearlInBrite Whitening Enhancer at home than by using a
product designed by PearlInBrite’s creator himself, Dr. Jan Linhart? This
enhancer gel acts as a supplement to your everyday toothpaste and eliminates
the need to wear whitening strips. It uses hydrogen peroxide to enhance your
toothpaste, and you don’t even have to brush separately! Simply apply the gel on top of your toothpaste before
brushing.
3.) Minimize Exposure to Substances that Stain
Coffee. Red Wine. Certain foods with
rich sauces. All the good stuff. While you don’t need to eliminate these from
your diet completely, minimizing your consumption of them can help prolong the
effects of your whitening treatment. After all, these are the foods and
beverages that can leave lasting stains. Smoking is another substance that
causes discoloration and yellowing of the enamel. If you do consume any of
these, we recommend brushing or using mouthwash soon after to minimize the
chance of lasting stains.
4.) Maintain Regular Dental Cleaning Visits
Regularly scheduled visits with your
dentist are necessary anyway to preserve the health of your teeth. But
receiving your cleaning at least twice annually from your dental hygienist can
help minimize any new stains accumulated since your last PearlInBrite
treatment.
5.) Consider Subsequent PearlInBrite Treatments
The results of PearlInBrite can last
for a long time, and can be prolonged even longer in patients who follow the
aforementioned tips. But the truth is that no whitening treatment is permanent.
The daily wear-and-tear we put our teeth through eventually catches up to us,
and we’ll eventually need to have our teeth whitened again. Fortunately, with
PearlInBrite’s exemplary whitening effects, this doesn’t have to happen often.
But if you’re noticing that your smile is losing a bit of the luster it had
after your first PearlInBrite treatment, consider contacting our office to
schedule another one. There’s nothing wrong with a little touch up.
As with your teeth’s overall strength and health, the whiteness
of your teeth can last for a long time if you take care of them properly. Daily
brushing, the use of dentist-recommended whitening products, and regular visits
to your dentist can make your PearlInBrite smile brighter for longer. Visit www.peralinbrite.com
to learn more about the system, and schedule your appointment today!
Porcelain veneers are an effective, long-term
solution for transforming discolored or misshapen teeth into a beautifully
white and perfectly aligned smile that will last for decades. The procedure
involves thin pieces of porcelain (veneers, or laminates) that are hand-crafted
by a lab technician into the shape of perfect teeth. The laminates are then
bonded to your natural teeth to correct the their imperfections and create an
authentic, uniform smile.
Orthodontic treatments such as Invisalign
or braces can straighten misaligned teeth, and
are important for improving your bite, jaw structure, or strength of your
teeth. However, they cannot correct chips, permanently stained, or misshapen
teeth. Teeth
whitening procedures can brighten your smile to an extent, but some
tooth discoloration cannot be corrected by these treatments, and the effects
are always temporary. Porcelain veneers are quick, easily applied by a restorative
dentist, and, when properly cared for, will last for years.
As with any dental procedure, cosmetic or otherwise, it is
important to discuss with your dentist whether or not the course of treatment
is right for you. Are you considering porcelain veneers? These seven
requirements might indicate that you’re an ideal candidate.
1.) Discolored teeth
If you have teeth with deep, tough
stains, traditional whitening procedures may not be enough to remove them.
Mottled teeth with lines or bands that leave the enamel rough collect plaque
and other debris that make stains more prominent. Laminates bond to the enamel
and cover over the unsmooth surface.
2.) Misshapen teeth
Some people have naturally misshapen
teeth, like incisors that curve at an odd angle or front teeth with ridges on
the ends. Porcelain veneers are smooth and uniform, creating the appearance of
aligned teeth that are all properly shaped.
3.) Fractured teeth
Fractured teeth are misshapen, not by
the natural development of your teeth, but by accidents or other factors that
actually break or crack your tooth. While it is important to seek the proper treatment for fractured teeth to prevent more
serious issues, you may still be left with a tooth that is noticeably
different. If this has happened to more than one of your teeth, you might
consider porcelain veneers to cover up traces of other dental work.
4.) A properly aligned bite
Crooked teeth are certainly a reason
that some people elect to receive porcelain veneers. However, porcelain veneers
are only an option for mildly misaligned teeth. People with crooked teeth that
result from issues with the formation of their jaw, or those who have a
seriously misaligned bite, require orthodontic treatment such as braces or
Invisalign.
5.) Healthy gums
Gum disease is a serious issue that
can cause various complications, and can even sometimes require surgery to
correct. If you have a history of gum disease, or believe you may be exhibiting
symptoms, consult with a periodontist to determine the proper course of
treatment. Gum disease can weaken your teeth and the surrounding bone, and
porcelain veneers would not be a solution.
6.) Healthy tooth enamel
Porcelain veneers are bonded to the
enamel of your teeth, and therefore require a strong enamel to support them. If
you have weakened enamel, your dentist will need to determine if your teeth are
strong enough for porcelain veneers.
7.) You don’t grind your teeth
Habitually grinding your teeth not
only weakens your enamel, which can preclude you from porcelain veneers, but it
also means that once you have veneers,
you may cause damage to them. If you use a mouthguard at night or are otherwise
seeking ways to avoid grinding your teeth, your dentist might still decide that
porcelain veneers are the answer, but if it is a chronic habit that causes
other issues for you, then you might not be a candidate.
Porcelain veneers are a lasting, affordable,
and quick cosmetic fix for imperfections in your teeth that prevent you from
having the winning smile you’ve always wanted. Speak with your dentist today to
see if your teeth require other forms of restorative treatment, or if porcelain
veneers are right for you.
Teeth grinding, or bruxism, is a fairly common occurrence that results when people clench their teeth and gnash them together in a grinding motion. Many people do this during the day, either subconsciously or as a habit. Sleep bruxism, however, occurs when people grind their teeth at night. It is just as common, though it has the potential to become more problematic.
While grinding your teeth on occasion is not a cause for concern, the repeated or habitual grinding of your teeth can lead to a variety of complications. When people grind their teeth at night, they do so in their sleep, and are not aware of it. Prolonged, unconscious teeth grinding is where issues often arise.
Symptoms and Effects of Teeth Grinding
How do you know if grinding your teeth is an issue if you do it during your sleep? You may be unaware that you’re doing it, but if it happens on a regular basis, you’ll start to notice certain symptoms. Some of these symptoms include:
● A dull, constant headache originating in the temples
● Teeth that are suddenly more sensitive to heat, cold, or sweetness.
● Soreness on your tongue or the inside of your cheeks, as people who grind their teeth often bite themselves.
● Tired or tight jaw muscles.
If you are experiencing any of these symptoms, consult with your dentist to determine whether or not you grind your teeth. Please keep in mind that many of these symptoms might be indicative of other conditions, which is why it’s important to confirm or rule out teeth grinding as the cause. During your regular dental checkups, your dentist will typically check for signs that you grind your teeth.
Grinding your teeth weakens your enamel. It can flatten or wear down your teeth, which causes issues with your bite, and if left untreated, you can potentially loosen or fracture a tooth. Lockjaw and other temporomandibular joint dysfunctions (TMD, or disorders of your jaw muscles) can result from chronic, repeated teeth grinding.
What Causes Teeth Grinding?
Doctors don’t have a full understanding of all the causes for grinding your teeth. Stress, anxiety, or even pure force of habit are some common causes. Teeth grinding is very common in childhood, and it can also be caused by sleeping disorders, such as sleep apnea. If your dentist believes your teeth grinding is caused by a sleeping disorder, or another psychological condition, he or she may refer you to a sleep specialist to determine the underlying causes that must be addressed before the teeth grinding can be alleviated. People with overbites or an abnormal alignment of their upper and lower teeth may also experience bruxism.
How to Prevent Teeth Grinding
There are different methods to keep yourself from grinding your teeth at night, and you and your dentist will determine the technique that is right for you. Here are five ways you can stop grinding your teeth.
1. Wear a mouthguard
Mouthguards are the easiest and most typical measures taken against teeth grinding. Your dentist will fit you with a custom plastic mouthguard that you wear every night to sleep. While you’ll probably still move your mouth during the night, the guard acts as a buffer by preventing your teeth from grinding against each other. The soft plastic keeps your teeth safe and prevents further weakening of the enamel.
2. Dental correction
In cases where your teeth grinding is caused by a dental problem, the proper procedure to correct the issue might be the right course of action. If you grind your teeth because of a dental misalignment, braces or Invisalign might gradually help you stop by improving the issue. If you have damages to your teeth that cause irregularities in the chewing surfaces, crowns could alleviate your teeth grinding.
3. Stress management
For many people, teeth grinding is an instinctual response to stress or anxiety. Oftentimes, if somebody is stressed at work, the subconscious anticipation of the next day’s probable stress can cause them to grind their teeth during their sleep the night before. While your dentist cannot recommend the method of stress management best suited for you, if your teeth grinding is determined to be a result of stress, seek out healthy forms of relieving stress that might help you sleep easier and grind your teeth less.
4. Avoid stimulating substances
Certain substances such as caffeinated beverages, or even alcohol, when consumed before bed can increase the frequency of teeth grinding.
5. Consult with a sleep specialist
If it is determined that you grind your teeth as a symptom of a sleeping disorder, you may need to consult with a sleep specialist to determine the proper treatment for the disorder. By addressing your sleeping issue at its source, the symptoms of the disorder, including your teeth grinding, should gradually be minimized.
Do you think you grind your teeth at night? If you experience any of the symptoms mentioned above, and have not been able to determine another probable cause, it’s possible that you do. Ask your dentist to examine you for signs that you grind your teeth before your symptoms get worth, and explore which preventative measures are right for you.
When it comes to orthodontic
treatment, the field of dentistry has come a long way. In the past, traditional
braces using metal brackets anchored to the teeth to correct misalignment or
crookedness was a patient’s only options. Metal braces are still a widely used
and highly effective method, but nowadays, patients can choose from a wide
array of alternatives depending on their individual needs, aesthetic
preferences, and budget.
Orthodontics has evolved to take discretion and appearance into
consideration, creating effective alignment solutions that patients can wear
without having to be self conscious. Porcelain
veneers, for example, are an excellent cosmetic solution for
patients with minor misalignment. For a substantial overbite or more serious
orthodontic issue, however, patients can consider iBraces,
which are smaller than traditional braces, and are anchored to the back of your teeth to be virtually
invisible.
One orthodontic treatment has become one of the leading
alternatives to braces. Invisalign, for adults or teens,
is a series of clear plastic trays that are molded specifically to your teeth
and fit over your teeth to align
them. They function in much the same way as traditional braces, with the
obvious benefit of being, well, invisible. Aside from the visual difference,
though, there are some functional differences between braces and Invisalign.
Let’s explore some of the major ones.
How Do Invisalign and
Braces Straighten Teeth?
If you have had braces in the past, or know somebody who has
braces, you’re familiar with the check ins every few weeks with your
orthodontist to tighten the braces. The wire that’s anchored to your teeth is
gradually tightened over the course of treatment, literally squeezing the teeth
together to straighten them. This must happen in the office, which is
beneficial in that it allows your orthodontist to closely monitor the progress
of your treatment.
Invisalign also works by applying incremental pressure to your
teeth to tighten them, however, it uses a series of plastic trays, or aligners,
to do this. While Invisalign aligners are molded to the shape of your teeth,
each is a slightly different size, following the natural progression of your
straightening process. Every subsequent tray is just a bit straighter, until
ultimately, your final tray is the shape of your perfectly straight smile.
Instead of tightening a wire like with regular braces, you simply change your
tray roughly every two weeks.
You must still meet with your orthodontist on a regular braces,
but changing trays can be done easily and conveniently at home. Typically, your
orthodontist will give you a few trays at a time to last you between visits.
Trays are numbered, and you wear them in numerical order.
How Do Invisalign and
Braces Affect Your Day-to-Day?
One of the clearest advantages of Invisalign over braces is
that Invisalign is removable. This means that daily activities like eating,
drinking, and brushing your teeth aren’t affected at all. In fact, you have to remove your Invisalign tray when
eating or drinking. But you can still eat whatever you want because there is
nothing obstructing your teeth. Optimal wear for your Invisalign tray is 22
hours per day, but this still allows you plenty of time to keep the tray out
while eating.
With braces, however, food can get caught in between the
brackets. You have to take extra care to brush after every meal to avoid a
buildup of plaque and bacteria from food particles that accumulate around the
the braces. Foods that are too hard or sticky can be difficult to brush away
from your braces, and can even potentially damage them. Because of this,
patients often avoid foods they once loved to avoid the hassle they cause for
their braces.
Speaking of brushing, your daily oral hygiene routine is
completely unaffected by Invisalign. While you should ideally be brushing more
(after each meal to properly clean your teeth before putting your tray back
in), the fact that you remove your tray for brushing means that you can brush
normally. When you wear braces, you have to take extra care to avoid damaging
the wire when you brush, and there are certain areas of your teeth that you’ll
miss altogether. This makes it difficult to be as thorough with your brushing
as you typically would without braces.
—
There are many factors to consider when choosing between
Invisalign and braces. Because Invisalign straightens teeth through the use of
trays and not the tightening of wires, your orthodontist has less direct
control over the movement of your teeth. Treatment may take longer, and there
are some orthodontic issues, such as overlapping teeth, that Invisalign alone
may not be able to correct. But with any course of treatment, consulting with
your orthodontist and learning as much as you can about your options will help
you make the decision that’s right for you.
It is well known that fluoride, an element found in most water
sources, has numerous dental benefits. It is essential to proper oral care.
Fluoride can strengthen teeth and prevent tooth decay by keeping the acid
produced by the bacteria in plaque from dissolving the enamel of our teeth. It
cannot restore teeth with cavities, but it can
prevent cavities, and it also reverses the early stages of tooth decay by
allowing tooth enamel to repair, or remineralize, itself. Fluoridated water,
toothpaste, mouthwash, and supplement pills are all sources of fluoride.
Proper fluoride intake is an important part of a well-rounded
dental health regimen. Infants and young children don’t require as much,
however, when carefully monitored, a child’s intake of fluoride is still a
beneficial and necessary part of their oral care.
Fluoride Intake for
Infants
Infants require the least amount of fluoride of any age group.
Fluoride supplements, which are usually prescribed when children live in an
area without fluoridated water, are not necessary for infants. For children
under six months of age, the water used to prepare a baby’s formula provides
sufficient fluoride. Baby formula generally contains fluoride already, with milk-based
formulas containing less fluoride than soy-based formulas. Because of this,
parents have the option of supplementing the level of fluoride contained in
baby formula by preparing their child’s formula with tap water or fluoridated
bottled water. If they want to limit their child’s fluoride intake, they can
use non-fluoridated bottled water.
Some parents also choose to breastfeed as a way to limit
fluoride intake. It should be noted, however, that breast milk contains only
very small trace amounts of fluoride, and a breast milk fed baby receives
virtually no fluoride exposure. Parents are advised to consult with a dentist
to determine how to ensure their infants receive the right amount of fluoride.
When baby teeth begin appearing, parents can brush their
child’s teeth with an infant toothbrush using water and a tiny smear of
toothpaste. Children’s teeth should be brushed this way until around age two.
Fluoride Intake for
Young Children
After the age of two, children begin brushing their own teeth,
thus regularly ingesting fluoride in their toothpaste. Past this age, most of
their fluoride intake comes from water, so children should only use a small
amount of toothpaste when they brush. A pea-sized amount is more than
sufficient, and children should always use a toothpaste that carries the ADA’s seal
of approval.
Under the age of six, children should not use mouth wash that
contains fluoride. Younger children have a tendency to swallow too much
toothpaste while brushing, and if they use mouthwash, there is a high
likelihood of them swallowing that as well. Parents should supervise young
children when they are brushing their teeth to ensure they are not swallowing
their toothpaste. It is around this age when, if a child lives in an area
without a fluoridated water supply, a dentist might prescribe fluoride
supplements to build their fluoride intake beyond toothpaste.
—
Fluoride is a pivotal part of maintaining proper dental health.
While fluoride intake needs to be carefully monitored in infants and young
children to avoid overexposure, parents should not be deterred from recognizing
the benefits. Speaking with a dentist or pediatric dentist is an excellent way
to learn more about caring for children’s teeth, and obtaining more information
about fluoride needs.
